Advanced Device-Based Technologies in Cosmetology: Safety and Clinical Protocols
Authors
Pysmenna Anna

Share
Annotation
This article provides a comprehensive overview of modern hardware techniques used in aesthetic medicine, such as laser, radiofrequency, ultrasound, and IPL light technologies. The focus is on the safety profile of these techniques, analyzing potential risks and methods for preventing and managing adverse events. Standardized clinical protocols are analyzed, which guide the choice of equipment and parameters based on the patient's skin type and individual features. The importance of following step-by-step algorithms for pre-procedure preparation and post-procedure rehabilitation is emphasized. The work highlights the critical importance of adhering to the principles of evidence-based medicine when incorporating innovative equipment into a cosmetologist's routine clinical practice, which is a prerequisite for achieving predictable, effective, and safe therapeutic outcomes.
Keywords
Authors
Pysmenna Anna

Share
Relevance of the study. The study is becoming particularly relevant due to the dynamic development of aesthetic medicine and the steady increase in patient demand for non-invasive and minimally invasive methods for correcting age-related changes and dermatological problems.
High-energy equipment is regularly appearing on the market, including ablative and non-ablative lasers, microneedle RF lifting systems, and high-intensity focused ultrasound (HIFU) devices. These technologies significantly expand the therapeutic capabilities of doctors. However, the use of such powerful physical factors inevitably involves the risk of iatrogenic complications, such as deep burns, persistent post-inflammatory hyperpigmentation, scarring of tissues, and exacerbation of chronic dermatoses.
In the context of active product promotion and a sometimes careless attitude to the rules of using equipment, there is an urgent need for a thorough systematization of the accumulated global clinical experience. An extremely important step is to create a unified evidence base confirming the safety of the technologies used. It is also necessary to implement strict, regulated protocols that will help minimize the likelihood of medical errors and ensure the predictability of aesthetic results.
The purpose of the study. The purpose of the study is to conduct a comprehensive analysis of the safety profile of modern hardware technologies used in cosmetology and the scientific systematization of standardized clinical protocols for their use.
The key objective of the work is to create clear algorithms for the personalized selection of physical exposure parameters based on skin phototype, aging morphotype and patient's medical history. In addition, the aim of the study is to develop effective strategies for the prevention and management of potential adverse events at all stages of treatment and recovery.
Materials and research methods. The research is based on a comprehensive multidisciplinary approach, which includes an in-depth retrospective analysis of modern Russian and foreign scientific literature on dermatocosmetology.
We collected most of the data through a systematic search in the international medical databases PubMed, Cochrane Library, Scopus, and eLibrary. We filtered the publications for the last ten years. In our work, we used methods of meta-analysis of the results of randomized clinical trials, cohort studies, and detailed reports on clinical cases associated with complications after hardware interventions.
A comparative analysis of the official clinical recommendations of the international aesthetic communities and factory manuals of leading manufacturers of medical equipment was also carried out. Methods of statistical processing of epidemiological data on the frequency and nature of side effects were used to identify objective patterns. This made it possible to develop reliable algorithms for the safe use of high-intensity hardware techniques in everyday clinical practice.
The results of the study. The evolution of cosmetic surgery began at the end of the 19th century and is closely related to the introduction of electricity into clinical medicine. The first significant breakthrough was made in 1891, when the French physiologist Jacques Arsène d'Arsonval discovered the therapeutic effect of high-frequency pulse currents. This discovery led to the development of the darsonvalization method, which continues to be used today to stimulate microcirculation and treat inflammatory skin diseases. During the same time, in 1875, the American ophthalmologist Charles Michel used direct galvanic current to destroy hair follicles in the treatment of trichiasis. This became the basis for electroepilation, a method that has since been widely used in cosmetic surgery.
During the first half of the 20th century, aesthetic medicine primarily borrowed techniques from classical physiotherapy. Techniques such as iontophoresis, galvanization, and vacuum massage were introduced into practice. These methods allowed for non-invasive stimulation of cellular metabolism and improved the transdermal absorption of topical medications.
A true technological revolution in aesthetic medicine took place in the second half of the 20th century thanks to the invention and application of laser radiation. Following the creation of the first ruby laser by Theodore Maiman in 1960, extensive research into the effects of focused light on biological tissue began.
A major event that altered the course of industry development was the publication of the theory of selective photothermolysis by Rox Anderson and John Parrish in 1983. This concept scientifically proved the possibility of targeting the destruction of specific cells containing melanin, hemoglobin, or water using light energy at a precisely defined wavelength, without causing thermal damage to surrounding intact structures. This discovery provided a powerful impetus for the development of specialized systems for laser hair removal, treatment of vascular pathologies, and pigmentation disorders.
In the 1990s, the first carbon dioxide and erbium laser devices for deep skin resurfacing were introduced on the market. These devices provided unprecedented results in reducing the appearance of wrinkles and scars, but they required long and difficult recovery periods for patients (Table 1).
Talitsa 1 - Ablative carbon dioxide lasers in cosmetology
|
Indications |
Advantages |
Disadvantages and risks |
|
|
|
Since the beginning of the 21st century, the development of medical technologies has taken the path of minimizing tissue injury and speeding up the recovery process. In 2004, a revolutionary fractional photothermolysis technology was developed, which allows microscopic areas to be affected on the epidermis and dermis, preserving healthy cells around them for accelerated regeneration.
At the same time, non-laser correction methods were actively developing. IPL broadband pulsed light systems for non-ablative photorejuvenation, as well as RF radiofrequency lifting devices that stimulate neocollagenesis through deep controlled heating of the dermis, have become particularly popular. The last decade has been marked by the widespread introduction of HIFU technologies for non-surgical SMAS lifting, cryolipolysis devices for modeling body contours, and microneedle radiofrequency exposure systems [1].
It should be noted that modern hardware cosmetology is a highly advanced branch of aesthetic medicine, where maintaining a balance between clinical effectiveness and patient safety is of utmost importance.
The global hardware cosmetology market is growing at a rate of 13-15% per year (CAGR), and is projected to exceed $18 billion by 2030. Over 70% of patients seeking aesthetic treatments prefer non-invasive hardware methods to plastic surgery. Approximately 45% of treatments today are performed using combined protocols (devices + injections) in order to maximize results [2].
The basis for successful work with laser, radiofrequency, and ultrasound systems is careful standardization of procedures and strict adherence to clinical protocols [4]. These protocols, developed based on the principles of evidence-based medicine, define every step of the doctor's interaction with the patient. They begin with collecting anamnesis and determining the phototype of the skin on the Fitzpatrick scale and end with the selection of optimal physical parameters of exposure and the appointment of proper rehabilitation care.
The safety of procedures at the level of the devices themselves is ensured with modern monitoring and feedback systems. Modern platforms have built-in sensors that constantly monitor skin temperature, tissue electrical resistance, and the quality of the manipulator's contact with the skin. This avoids thermal burns caused by light and laser exposure. Multi-stage systems, such as contact sapphire glasses, dynamic cryogenic spraying, or powerful cold air blowing, are used to cool the skin.
To protect the vision of the doctor and the patient, special glasses are used that block radiation of a certain wavelength. In recent years, manufacturers have been actively implementing artificial intelligence algorithms. These algorithms automatically analyze the level of melanin and skin hydration, which allows the doctor to choose safe energy parameters and minimize the risk of error.
Clinical protocols are clearly delineated depending on the physical energy used. When working with HIFU, the gold standard of safety is the use of real-time imaging. This allows the doctor to accurately determine the depth of the musculo-aponeurotic layer (SMAS) and prevent accidental damage to large blood vessels or nerve nodes.
The protocols of microneedle radiofrequency lifting involve the use of strictly individual sterile nozzles with insulated needles. These nozzles conduct electric current only at certain depths, for example, 1.5 or 3.0 mm, reliably protecting the surface of the epidermis from overheating. In laser therapy and when working with broadband light (IPL), the key rule is to accurately observe the time of thermal relaxation of tissues. Before full-scale treatment of the area, it is necessary to conduct test flashes to assess the immediate erythematous skin reaction (Fig. 1).
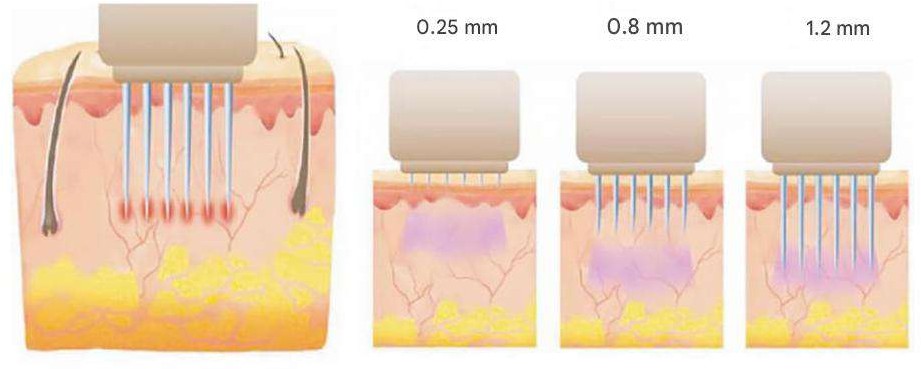
Fig. 1 – Operation diagram of needle RF lifting
The safety of medical practice begins with careful patient selection. It is important to take into account absolute and relative contraindications, such as cancer, pregnancy, the presence of pacemakers, and acute dermatological conditions. Modern clinical guidelines increasingly use combined protocols that involve the consistent application of various physical factors within a single course.
One of the classic examples is the combination of none-ablative fractional photothermolysis and injectable biorevitalization. Another example is cryolipolysis combined with hardware lymphatic drainage. This approach allows doctors to use lower and gentler energy parameters for each device. This reduces the risk of post-traumatic hyperpigmentation and scarring. As a result, the aesthetic result becomes more pronounced, and the period of social rehabilitation of the patient is shortened.
Clinical results in numbers:
- SMAS lifting (ultrasound) – reduces the area of the skin flap by 15-25% in one procedure, and the visual lifting effect is enhanced within 3-4 months.
- Microneedle RF lifting – reduces the depth of skin wrinkles by 30-40% and reduces the severity of post-acne scars by 40-50% after a course of 3-4 procedures.
- Cryolipolysis is the hardware cooling of fat cells, which ensures the irreversible destruction of 20-25% of the local adipose tissue in the treatment area in one session.
- Laser hair removal (diode and alexandrite) – guarantees the removal of 85-95% of hair in the active growth phase in a course of 6-8 visits.
- Laser resurfacing (CO2) – renews up to 20-30% of the epidermis surface in one pass, significantly accelerating cellular metabolism.
Comparative analysis with injections and plastic surgery:
- The risk of complications when using hardware cosmetology is less than 1.5-2%. Most often, this is transient erythema or hyperpigmentation, which may occur if the procedure protocol is not followed. For comparison, in injectable cosmetology, the risk is 3-5% (for example, ischemia or granulomas), and in plastic surgery – 5-10%.
- The recovery time after hardware procedures ranges from 0 to 7 days, while surgical intervention requires from 14 to 60 days of full-fledged social rehabilitation.
- The life cycle of the client (LTV) using hardware techniques is 35-40% higher than with injection methods, since the latter require course application (for example, for laser hair removal, photorejuvenation, or body shaping).
Clinical studies confirm that the combination of hardware heating (e.g., RF) and injections (polylactic acid or collagen) can increase dermis density by 40-50% more effectively than using these methods separately. Over the past five years, there has been a significant increase in patients aged 25 to 30 who resort to preventive hardware procedures such as IPL therapy and Hydrafacial. The use of original certified devices approved by the FDA, CE, and Roszdravnadzor reduces the risk of adverse events by 90% compared to more affordable, non-certified analogues [5].
It is important to note that, despite impressive clinical results, the use of high-energy hardware technologies in cosmetology is fraught with significant difficulties. The main one is the insufficient level of specialist training. Deep academic knowledge in tissue physics, topographic anatomy, and dermatology is required to work with modern laser, radiofrequency, and ultrasound medical platforms. This necessitates continuous skill improvement and professional development for operators [6].
Unfortunately, in practice, specialists without specialized medical education or those who have completed only superficial commercial training often perform procedures. Failure to critically assess anamnesis, accurately determine tissue depth, and correctly select energy density can lead to serious complications such as deep thermal burns, subcutaneous fat atrophy, facial nerve damage during SMAS lifting, and the formation of persistent keloid scars.
Another significant problem in hardware cosmetology is the uncontrolled distribution of counterfeit and non-certified medical equipment. Many institutions, aiming to minimize capital costs, purchase shadow copies of premium devices that do not undergo rigorous technical and clinical trials.
Important safety systems, such as tissue impedance feedback and dynamic cooling of the epidermis, are missing or malfunctioning in such devices. Due to unstable pulse generation and unpredictable energy dissipation in tissues, the use of standardized treatment protocols becomes impossible. The situation is aggravated by the widespread practice of saving on consumables. Clinics use hacked programs to reuse disposable nozzles and insulated needles. This not only reduces clinical efficacy due to degradation of the conductors but also seriously violates infection safety protocols.
An important aspect that causes problems in the interaction between the doctor and the patient is the concealment of information and non-compliance with the rehabilitation regime. Patients often do not report the presence of absolute contraindications, such as fresh tanning, taking systemic retinoids, antidepressants, or photosensitizing antibiotics. The use of light or ablative technologies against the background of such conditions can lead to unexpected consequences, such as hyperpigmentation, persistent erythema, or serious violations of the skin regeneration process.
The situation is significantly complicated by aggressive marketing and promises of immediate results broadcast on social media. This leads to the formation of unrealistic expectations among patients, which puts psychological pressure on doctors. Doctors are then pushed to overestimate energy parameters to achieve instant results, blurring the line between therapeutic damage and irreversible tissue destruction.
We believe that solving the issue of insufficient qualifications requires government regulation and reform of postgraduate medical education. It is essential to introduce mandatory certification for each specialist, with regular confirmation of his or her practical skills on high-energy equipment.
The training should go beyond superficial commercial training provided by distributors and include in-depth academic study of the physics of hardware impact techniques, as well as mandatory cadaver practice to ensure a thorough understanding of topographic anatomy. Legislative consolidation of the right to perform aggressive hardware procedures solely for doctors who have undergone specialized retraining in cosmetology would minimize the risk of serious iatrogenic complications.
To eliminate the counterfeit medical device market, it is necessary to implement a mandatory, statewide digital labeling system that tracks medical devices from their production to the end user. This system should include end-to-end traceability, ensuring that all devices are authentic and safe for use.
Original medical device manufacturers should also take steps to protect their products by implementing hardware-level encryption and RFID tags based on chips. These technologies can prevent unauthorized use of devices, such as using gray market or hacked devices, and ensure that devices are not used multiple times after they have been disposed of. Regular technical audits by supervisory authorities, with the ability to confiscate non-compliant devices, will help ensure that clinics comply with infection safety standards and the predictability of treatment outcomes.
Overcoming communication barriers with patients and minimizing the negative effects of aggressive marketing can be achieved through strict standardization of legal support for medical procedures. The introduction of detailed digital medical history checklists integrated with unified electronic medical records to automatically verify prescriptions for antidepressants, retinoids, or photosensitizers, will eliminate the risk of withholding important information.
Expectation management should be based on ethical codes and a legal ban on the publication of unscrupulous advertising that promises instant results without proper rehabilitation. The use of objective hardware skin analysis systems before and after procedures can help relieve psychological pressure on doctors, prevent dangerous overestimations of energy parameters in order to achieve instant lifting, and focus on safe physiological tissue regeneration protocols.
Conclusions. Modern hardware cosmetology is a highly intelligent field of aesthetic medicine, where the effectiveness of treatment directly depends on strict compliance with safety rules and the use of scientifically proven clinical protocols.
The rapid development of laser, radiofrequency, ultrasound, and photosystems opens up new horizons for noninvasive rejuvenation, tissue repair, and treatment of dermatological diseases. However, as the equipment becomes more powerful and the physical parameters of the impact become more complex, a deep understanding of the basics is required.
Fundamental knowledge about the biophysics of optical and acoustic waves, topographic anatomy, and cellular response mechanisms is a cornerstone for preventing serious complications such as thermal damage, scarring, and persistent dyspigmentation.
The guarantee of patient safety today relies on a three-pronged approach, including the use of legally certified equipment, continuous professional development for doctors, and strict adherence to personalized protocols that consider the patient's morphotype, skin type, and medical history. The industry's transition from aggressive marketing to evidence-based principles, the introduction of prediagnostic hardware methods, and transparent communication form a strong foundation for successful treatment.
Long-term success will depend on a combination of innovative engineering solutions, rigorous government regulation, ethical standards, and deep medical expertise. This will allow us to achieve predictable and aesthetically pleasing results while maintaining patient health and safety.
References:
- Chebanova I. A Critical Evaluation of Laser-Based Technologies in Modern Cosmetology: Clinical Efficacy, Procedural Benefits, and Associated Risks //Universal Library of Innovative Research and Studies. – 2025. – Vol. 2. – No. 1.
- Chuhraev N. et al. Hardware methods in cosmetology. Programs of face care //Medical Innovative Technologies, Kiev, Ukraine Radomska Szkoła Wyższa w Radomiu, Polska Radom University in Radom, Poland. – 2016. – pp. 32-36.
- Krupskyi O., Stasiuk Y., Huk O. Improving business efficiency in cosmetology institutions //Innovative economy. – 2024. – No. 3. – pp. 92-102.
- Skiba R. Advances in Cosmetology: Beauty Therapy Technology, Treatments, Sustainability, and Holistic Wellness. – After Midnight Publishing, 2025.
- Solianik M. Adaptation of international standards of education in the field of cosmetology to the national context of personnel training // Pedagogical Academy: scientific notes. – 2025. – No. 17.
- Rudyeva A. D. Modern terms in the beauty industry //Experientia est optima magistra. – 2022. – pp. 383-387.


